When a child says, “I am the worst at math” after one bad quiz, most parents try to talk them out of it. “That is not true. You did fine on the last one.” It rarely works. The thought sticks anyway.
Cognitive-behavioral therapy for kids, often shortened to CBT, offers children a different way to handle thoughts like that one.
It does not argue with the child. It teaches them how to question their own thinking and pick a more useful response.
CBT is also the most studied talk therapy in childhood mental health. That matters because it means parents are not guessing whether the approach works. Researchers have studied this for over four decades.
This guide explains how CBT for kids works, what a typical session looks like, what the research says about outcomes, and where the limits lie. The goal is honesty, not hype.
What is Cognitive Behavioral Therapy?
CBT is a short-term talk therapy built around one simple idea. Thoughts shape feelings, and feelings shape actions. Change the thought, and the feeling and behavior usually change with it.
For example:
- A child sees a classmate frown at lunch.
- Thought: “She hates me.”
- Feeling: sadness, then anger.
- Action: sits alone, refuses to talk for the rest of the day.
A CBT therapist would help that child notice the thought, ask whether there are other reasons the friend might have frowned (maybe she had a headache), and pick a thought that better fits the facts.
The feeling shifts. The behavior follows.
Quick History Bite: Aaron Beck developed CBT in the 1960s for adults with depression. Researchers later adapted it for kids and teens. The American Psychological Association now lists CBT as the most evidence-supported talk therapy for childhood anxiety, depression, OCD, and PTSD. |
CBT is one branch of behavioral therapy. The two terms overlap. Behavioral therapy looks at actions. CBT adds the thinking layer. Both are part of the same family.
How CBT Sessions Work for Children?
A real CBT session looks more like a conversation with worksheets than a deep emotional talk. Kids are usually surprised by how casual it feels.
Session length: Most sessions run 45-50 minutes.
Total course: 6 to 20 sessions for most kids, according to the team at Manhattan Psychology Group. Anxiety and OCD often need more. Simple cases need fewer.
Format:
- Individual: just the child and the therapist
- Group: a small group of kids working through similar issues
- Parent-involved: parent joins parts of each session, especially for younger kids
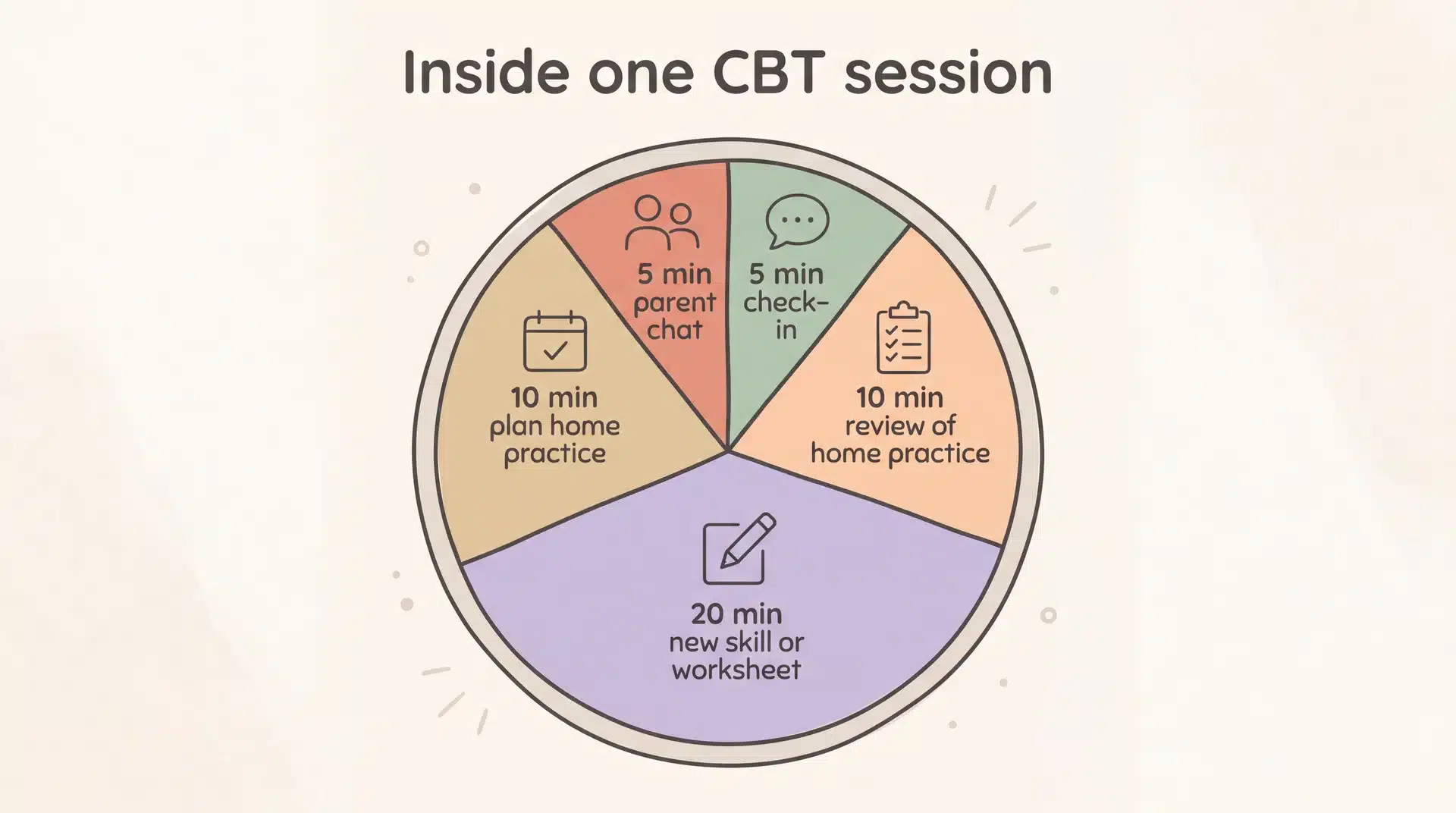
A typical CBT session usually breaks down like this:
| Time | What happens |
| First 5 minutes | Quick check-in on how the week went |
| Next 10 minutes | Review of last week’s home practice |
| Middle 20 minutes | New skill or topic, often with a worksheet, drawing, or role-play |
| Last 10 minutes | Plan home practice for the coming week |
| Final few minutes | Brief chat with the parent about progress |
The structure stays the same most weeks. Kids settle into it fast and often start asking for their favorite tools by name.
Core CBT Techniques Used with Kids
Therapists use a few core tools. Each one targets a specific thinking or behavior pattern.
1. Cognitive Restructuring: The child writes down a worry, then tests it against real facts. Healthline gives the example: “I stink at soccer. I am a total loser” becomes “I am not the best at soccer, but I am good at art and math.”
2. Exposure Work: For fears and anxiety, the therapist guides the child to face the feared thing in small steps. A child afraid of dogs might first look at a photo, then a video, then meet a dog from across a room, then closer.
3. Modeling: The therapist acts out a tricky situation, like saying no to a bully, and the child copies. Then the child tries their own version.
4. Behavioral Activation: Mostly used for depression. The child schedules small enjoyable actions, like 10 minutes of drawing, even when they do not feel like it. Action comes first. The mood often follows.
5. Relaxation and Grounding: Deep breathing, muscle-tension and release, and the five-senses grounding exercise. These are simple skills the child can use anywhere.
6. Thought Records: A worksheet where the child writes the situation, the thought, the feeling, and a more balanced thought.
Different kids click with different tools. A good therapist tries several and keeps what works.
Conditions CBT Effectively Treats in Children
CBT has been tested for almost every common childhood mental health concern. Some areas show strong results. Others show only modest gains. Both pictures matter.
Strong Evidence
- Childhood Anxiety Disorders: CBT is the only psychological treatment classified as evidence-based for anxiety in children, according to multiple reviews summarized in Global Healthcare Magazine.
- OCD: A specific form called Exposure and Response Prevention (ERP) is the standard treatment. The National Institute of Mental Health funded long-term studies on this in the early 2000s, and the results held up.
- Depression: CBT works well for mild to moderate childhood depression. Severe cases often need a combination of CBT and medication.
- Trauma and PTSD: A version called Trauma-Focused CBT (TF-CBT) is the recommended first treatment for children who have lived through abuse, loss, or major events.
Moderate Evidence
- ADHD: CBT helps with thinking patterns and self-control. It works best when combined with parent training and, in some cases, medication.
- Conduct Problems and Aggression: A 2021 review in Clinical Child and Family Psychology Review by Matthys and Schutter found CBT effective for conduct problems, but with effect sizes in the small-to-medium range. The authors suggest the field should focus more on emotion recognition and decision-making skills to improve results.
Where CBT is Not the First Choice?
|
What the Research Says About Effectiveness?
Most parents do not have time to read clinical trials. Here are the bottom lines:
Childhood Anxiety: Around 60 to 70% of kids show meaningful improvement after a full course of CBT, based on meta-analyses cited by the American Psychological Association.
Depression in Teens: CBT alone helps about half of teens with mild to moderate depression. The combination of CBT and medication helps more.
OCD: ERP-based CBT helps about two-thirds of kids and adolescents, based on the long-term follow-up of NIMH-funded trials.
Conduct Problems: Effect sizes are smaller. Matthys and Schutter (2021) noted that improvements are real but modest, and combining CBT with parent training gives the best chance of lasting change.
Long-Term Outcomes: Skills learned in CBT tend to stick. Many kids continue to use the techniques years after therapy ends, though booster sessions sometimes help during major life shifts.
The research is good, not perfect. Clinicians keep refining the methods. Parents who read older books or websites should know that the field has changed significantly in the last decade.
At What Age Can a Child Start CBT?
Traditional CBT works best for kids who can think about their thinking. That usually starts around age seven.
Below the age of seven, therapists adapt the work heavily. Younger children get:
- Drawings instead of worksheets
- Stories and puppets instead of thought records
- Heavy parent involvement
- A focus on behavior more than thoughts
The American Academy of Pediatrics recommends parent-training programs for children under 5 with behavioral issues. Direct CBT becomes a stronger fit later.
By the teen years, CBT looks closer to the adult version. Teens use full thought records, do their own exposure work, and often handle most of the session without a parent in the room.
| Age | What CBT looks like |
|---|---|
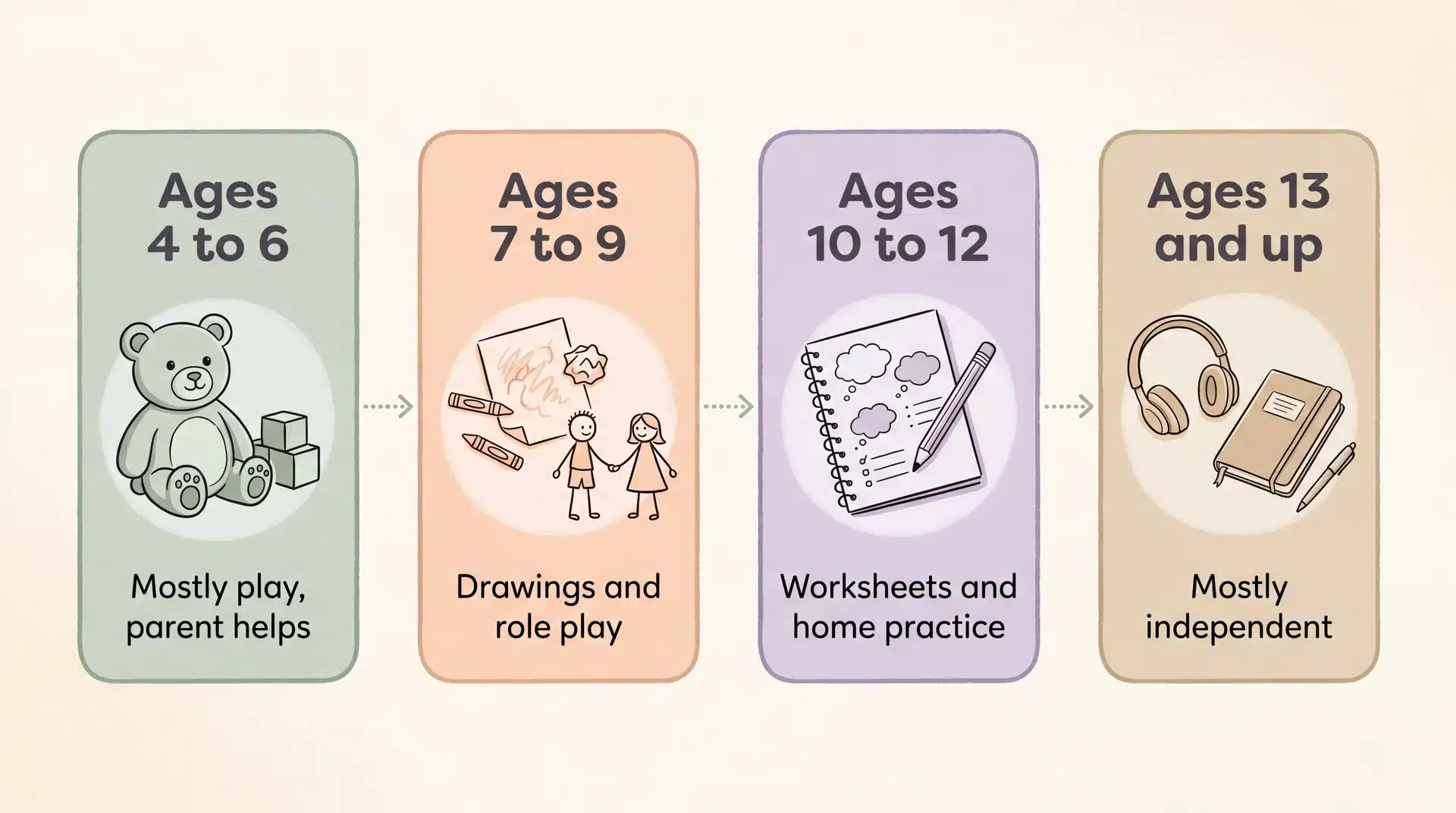
| 4 to 6 | Mostly play-based, the parent does most of the practice |
| 7 to 9 | Drawings, simple worksheets, lots of role-play |
| 10 to 12 | Standard worksheets, the child does home practice |
| 13+ | Adult-style CBT, mostly independent |
How Parents Can Support CBT Skills at Home?
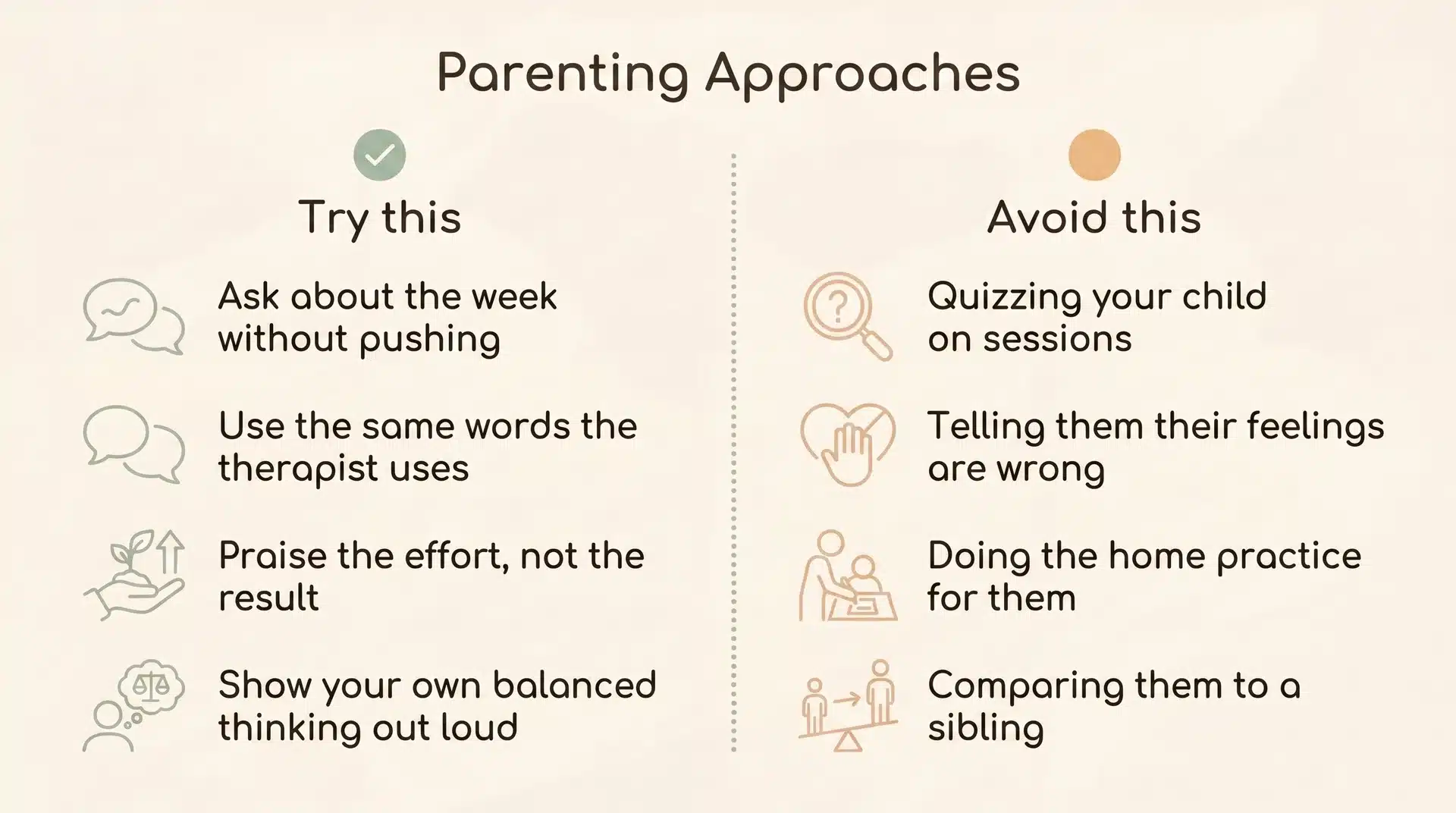
CBT only works as well as the practice between sessions. The therapist gives the tools. The home is where the tools get used:
1. Ask about the week’s home practice without pushing:
What did you work on this week? lands better than. Did you do your worksheet?
2. Use the same language the therapist uses:
If the therapist calls anxious thoughts “worry monsters,” you call them that too.
3. Praise effort, not outcome:
You tried something hard today; it matters more than if you did it perfectly.
4. Model your own balanced thinking out loud:
Kids copy how their parents handle stress.
5. Avoid rescuing:
If your child is afraid to order their own ice cream, let them try, even if they fumble. Anxiety shrinks when kids practice facing it.
What to Avoid?
|
Personal Note: The goal is to be the assistant coach. The therapist is the head coach.
CBT Compared to Other Forms of Child Therapy
Parents often ask how CBT stacks up against other options of child therapy.
CBT vs Play Therapy: Play therapy is most effective for younger kids who cannot yet talk through their feelings. CBT needs more verbal and thinking skills. Many therapists blend the two for kids in the seven to nine range.
CBT vs Dialectical Behavior Therapy (DBT): DBT is built on a CBT foundation but adds skills for handling intense emotions. It is mostly used for older teens with self-harm or extreme mood swings.
CBT vs Family Therapy:Family therapy treats the family as the unit. CBT treats the child as the unit. Some families need both.
CBT vs Medication: Medication can help with severe symptoms. CBT teaches skills that last. Many treatment plans include both, especially for moderate-to-severe cases.
Conclusion
CBT works because it gives children real tools. It also works because the tools transfer.
The breathing technique a nine-year-old learns in a therapy office shows up later as a teenager handling exam stress, or as an adult facing a tough conversation.
That said, CBT is not the right fit for every child. Younger kids, kids with severe trauma, and kids who need a body-based or play-based start often do better with another approach.
The research is detailed about what CBT can do and just as clear about where it falls short.
If your child is anxious, depressed, struggling with OCD, or working through a hard life event, CBT is worth a conversation with a licensed child therapist.
Ask about the research base. Ask how they adapt to your child’s age. The right starting point is the one that fits the child, not the one that sounds best on a website.
Frequently Asked Questions
Can My Child Do CBT Online?
Yes. Telehealth CBT works well for older kids and teens. Younger children often focus less on a screen, so in-person sessions usually go better for them.
What Are the Negatives of Cognitive Behavioral Therapy?
CBT requires verbal and thinking skills, weekly homework, and short-term emotional discomfort during exposure work. It also does not address deeper trauma without specific adaptation.











