Every parent has had the same quiet thought at some point. “Is this just a phase, or is something actually wrong?”
You watch your child melt down again over something small. You see them pull away from friends.
You wonder whether you are overreacting or have been ignoring something for too long. That doubt is real. And it deserves a real answer.
This guide walks you through the actual signs that a child might need behavioral therapy. You will see what counts as typical kid behavior, what crosses into red flag territory, and what to do next without panic.
What is Behavioral Therapy for Children?
Behavioral therapy is a type of mental health care that helps kids change unwanted behaviors and build better coping skills. It is structured. It is short-term in most cases.
And it has decades of research behind it from groups like the CDC and the American Academy of Child and Adolescent Psychiatry.
Adults often work through their problems by talking. Kids do it differently. They use play, drawing, stories, and movement. A trained child therapist meets the child at their level, not the other way around.
Behavioral therapy is also a broad umbrella term. Several methods sit under it. Some focus on the child alone. Others train the parent to respond differently at home.
The right one depends on age, the issue, and what the family can support. Behavioral therapy is also one of several approaches to child therapy
Signs Your Child May Need Behavioral Therapy
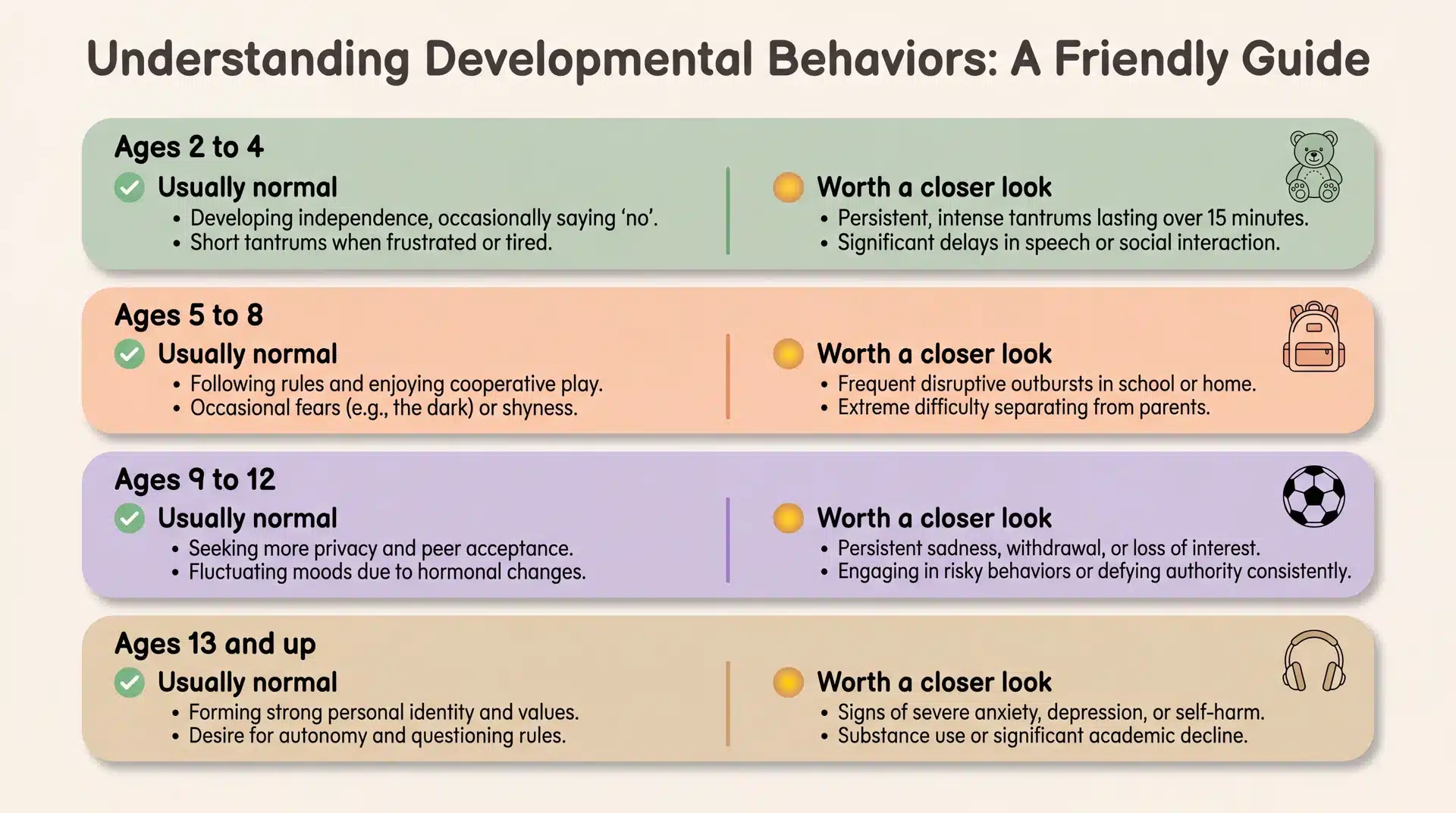
This is the part most parents actually search for. Below are the clearest signals from clinicians and pediatric researchers:
1. Tantrums or meltdowns are much more severe than peers’: All kids have outbursts. The Child Mind Institute reports that preschoolers who get kicked out of daycare or playdates over their behavior often need early intervention.
2. Refusal to follow instructions even after consequences: Therapists call this passive non-compliance. When you tell your child something six or seven times in a row, every day, that is more than ordinary stubbornness.
3. Sudden mood changes or social withdrawal: The Cleveland Clinic flags this as one of the strongest signs. A child who pulls away from family, friends, and activities they used to love is asking for help in their own way.
4. Self-harm signals: In young kids, this can look like head-banging, biting themselves, or digging nails into skin. In older kids and teens, cutting and verbal threats are clear red flags. Take these seriously every single time.
5. Trouble at school that does not match your child’s ability: Slipping grades, falling out with friends, and refusing to go to school can all point to a mental health issue, not a learning one.
If three or more of these match what you are seeing at home, that is a strong reason to call your pediatrician.
| Normal Behavior vs a Red Flag Most parents do not need a clinical degree to spot trouble. They need a simple filter. Use these four questions when you feel unsure.
|
The two-week rule:if sleep, eating, mood, or hygiene change for longer than two weeks, call your pediatrician.
How Behavioral Therapy Helps Children’s Mental Health?
Behavioral therapy works because it teaches the child a new pattern rather than just talking about the old one. The CDC notes that early treatment reduces the likelihood of more serious problems later in life.
That includes school failure, friendship trouble, and adult mental health issues.
Here is what the research and clinical guidelines tell us behavioral therapy can do, and which conditions respond well to it:
| What Behavioral Therapy Improves | Conditions it Helps Treat |
|---|---|
| Lower anxiety and depression symptoms | ADHD |
| Better self-control during big feelings | Anxiety disorders |
| Fewer fights and meltdowns at home | Depression |
| Better focus at school for kids with ADHD | OCD (obsessive-compulsive disorder) |
| Stronger coping skills after trauma, loss, or major change | Oppositional Defiant Disorder (ODD) |
| Better social skills and friendships | Conduct Disorder |
| Higher self-confidence | Autism-related behaviors |
| Early help reduces adult mental health issues | Trauma and PTSD |
The American Academy of Pediatrics specifically recommends behavior therapy as the first treatment for ADHD in children under six. Medication comes later, if it is needed at all.
Common Approaches Used in Behavioral Therapy
Several methods sit under the behavioral therapy umbrella. Here is the short version of the most common ones:
Cognitive Behavioral Therapy(CBT): The child learns how thoughts shape feelings, and feelings shape actions. Best for ages seven and up with anxiety, depression, OCD, or trauma. Sessions usually run for 6 to 20 weeks.
Parent-Child Interaction Therapy (PCIT): The therapist coaches the parent in real time, often through an earpiece, while the parent plays with the child. Best for ages 2 to 7 with disruptive behavior. NYU Langone uses this approach widely.
Applied Behavior Analysis (ABA): Often used for kids on the autism spectrum. Focuses on teaching new skills with positive reinforcement and clear feedback.
Behavior management training for parents: Parents learn how to set rules, praise specific actions, and apply consistent consequences. CHADD recommends this for children with ADHD.
Each method works differently and fits different kids.
The therapist will pick the best match after the first assessment. Some children also benefit from a treatment planthat includes other forms of therapy alongside their parents.
What to Expect in Your Child’s First Sessions?

Most parents get nervous about the first appointment. Here is what usually happens.
The Intake Call (15-30 minutes): You speak with the therapist before your child does. You share concerns, your child’s history, and what is going on at school. You can also ask any questions about the therapist’s training.
The First Session (45-60 minutes): The therapist meets your child. They might play, draw, or talk casually together. The point is to build trust, not start fixing anything yet.
Sessions Two and Three: The therapist sets goals with your child and you together. Many therapists will ask you to step into part of these early sessions.
Frequency: Most kids start with one session a week. Some need more, some less.
Total Length: Manhattan Psychology Group and other clinics report that most courses run for 6 to 20 sessions. Trauma cases often run longer.
Parent Involvement: You will likely attend some sessions, do home practice, or read short materials. The American Academy of Child and Adolescent Psychiatry says parent involvement is what makes therapy stick.
How to Find a Qualified Child Behavioral Therapist?
The credentials to look for are:
- Licensed Clinical Psychologist (PhD or PsyD)
- Licensed Clinical Social Worker (LCSW)
- Licensed Marriage and Family Therapist (LMFT)
- Board Certified Behavior Analyst (BCBA) for ABA-specific work
Always confirm that the therapist works with children. Adult therapy and child therapy are different jobs.
Five Questions to Ask on The Consult Call

- What training do you have in working with kids my child’s age?
- What approach do you use, and why does it fit our concern?
- How will you involve me as the parent?
- How do we measure progress?
- What happens if it is not working after a few sessions?
Free or Low-Cost Options
- School counselors are often the first stop and cost nothing.
- Community mental health centers offer sliding-scale fees.
- Your child’s pediatrician can refer you and may run a basic screening.
- University training clinics often charge less than private practices.
- Employee Assistance Programs through your job sometimes cover several free sessions.
Red Flags in a Provider
- They promise quick fixes
- They do not want to involve you
- They cannot explain why they use a specific method
- They blame the child for not making progress
Supporting Your Child Outside Therapy
Therapy works best when the home reinforces it. A few habits help.
1. Praise specific actions, not the child as a whole: “You shared that toy without being asked. That was kind.” This works better than “You are such a good kid.”
2. Keep routines steady: Sleep, meals, and bedtime should run on the same clock most days. Kids in therapy especially need this kind of stability.
3. Talk about therapy without shame: Frame it the way you would frame a tutor. The therapist is a coach for big feelings.
4. Watch your own responses: Kids copy how you handle stress. If you can stay calm during a meltdown, that lesson lands.
5. Stay in touch with the therapist: Most therapists welcome a quick email or note. Share what you are seeing at home, especially if something new comes up.
Conclusion
If you started this article wondering if this is just a phase, you are already doing the right thing. Listening to that gut feeling matters.
Use the filters above. Look at duration, intensity, impact, and how many parts of life are affected.
If three or more of the signs match what you are seeing, talk to your pediatrician this week. They can refer you to a child therapist or run a quick screening on the spot.
You are not overreacting. And you are not failing your child. Helping a child early is one of the most useful things any parent can do.
Frequently Asked Questions
At What Age Can a Child Start Behavioral Therapy?
As young as two for parent-training models like PCIT. Direct child therapy usually starts around age four for play-based work, and age seven for traditional CBT. (Source: NYU Langone, CHADD)
What is the Difference Between a Child Psychologist and A Child Therapist?
A child psychologist holds a doctorate (PhD or PsyD) and can run formal testing. A child therapist may be a social worker (LCSW) or counselor (LMFT) without a doctorate. Both can do therapy. Only psychologists can run formal psychological testing in most states.
Can My Child Benefit from Therapy if There is No Diagnosis?
Yes. A child does not need a diagnosis to benefit from therapy. Many kids see a therapist for stress, family changes like divorce, or social struggles. Insurance coverage may be different without a diagnosis, so check first.







